 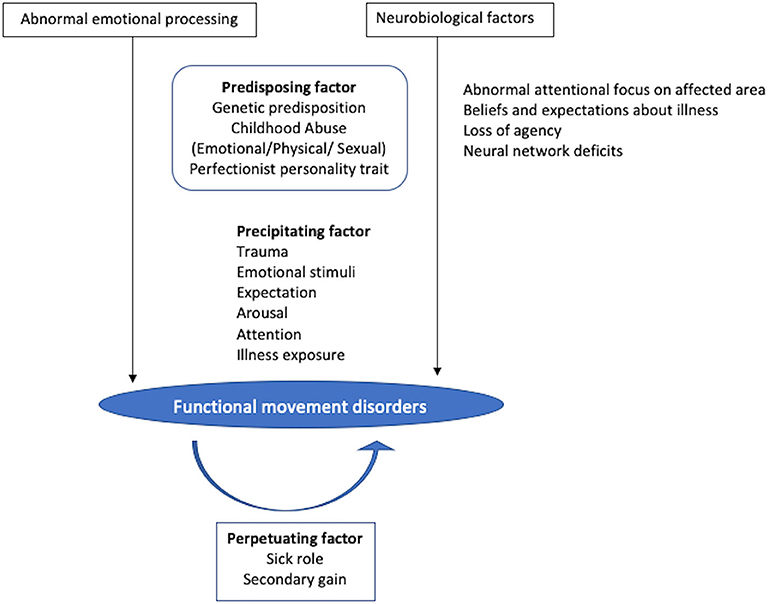 
Furthermore there is some evidence that these changes might be related to stressful life events in some people 4 (see Fig 2). Experiments looking at brain activity in FND (using ‘functional neuroimaging’ brain scans) suggest alterations in the activity of areas of the brain responsible for arousal and emotional processing, such as the amygdala (see Fig 1), and this might interfere with areas of the brain involved in initiating or planning movement such as the SMA (supplementary motor area) 1,2,3. There is also growing evidence that emotions, and abnormalities of its processing, might be involved in causing FND, at least for some patients. This experience can then become a form of ‘medical trauma’, taking on a life of its own, and potentially feed a cycle of symptoms and stress. Furthermore, many patients can feel stigmatized by healthcare professionals because of their FND diagnosis as the condition is so poorly understood by many healthcare professionals – this lack of understanding can become a significant roadblock in their care. However, it has become clear that there are many patients for whom this is not the case – although psychological factors might still be relevant in such patients as they can develop significant distress, and even depression, as a result of living with severe and chronic disorder such as FND and in such cases this can be helped by psychological treatments. 
stressful life events either before symptom onset or in the more distant past) might be relevant to the development of FND. Traditional theories of FND propose that psychological factors (i.e. Psychological factors, and therefore psychological treatments, can be important to consider in FND. Tim Nicholson (Maudsley Hospital and Institute of Psychiatry Psychology & Neuroscience, King’s College London, UK) Obtaining Your Medical Records in the UK.Research – Dissociation and Interoception in FND.Research – Occupational Therapy Consensus Recommendations for FND.Research – Functional Neurological Disorder.Life Events and Escape In Conversion Disorder.A preliminary investigation of sleep quality in FND.Neural Correlates of Recall of Life Events In Conversion Disorder.Impaired Self-Agency In Functional Movement Disorders: A Resting State fMRI Study.Several features can point to a FMD diagnosis. Physical exams, neuroimaging, and laboratory data usually do not explain FMD symptoms. The cause of the movements is not clear. Sometimes, they seem to be a reaction to stress. However, stressful events do not need to be present for a child to have FMD. Myoclonus appears as jerky limb or trunk movements. FMD can also include tics, speech problems, and more. Dystonia appears as spasms, abnormal posture, or twisting of arms and legs, torso, head, or combination of different body parts. There are three common abnormal movements that appear in FMD. FMD is also known as psychogenic movement disorder and falls under the umbrella of “functional neurological disorders.” There may or may not be a psychological cause present. FMD movements are not caused by something physically wrong with a patient’s brain, spinal cord, or muscles. In functional movement disorder (FMD), a child has abnormal, involuntary body movements. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
